Case series
- USA: 7 patients with allergic FRS that progressed to an invasive form (Ma et al, 2020)
- Saudi Arabia: 17 patients with chronic invasive FRS (Alotaibi et al, 2020)
- Iraq: 9 patients withrhinocerebral mucormycosis (Balai et al, 2020)

Factsheet
| NAMES Invasive fungal rhinosinusitis (fulminant fungal sinusitis) |
| DISEASE Presents with antibiotic-resistant fever, nasal discharge, stuffiness, ulceration or eschar of nasal mucosa, epistaxis, periorbital swelling, proptosis and/or visual impairment, facial pain and/or maxillary tenderness, black necrotic lesions or perforation of nose or hard palate and facial paralysis. In children, proptosis or eye muscle entrapment is common. Fungal invasion is usually found within the nasal cavity (~90%), typically at the middle turbinate. The infection is difficult to diagnose early but should be suspected when a neutropenic patient or uncontrolled diabetic develops persistent fever without a known source, symptoms of rhinitis or sinusitis, cutaneous findings over the nose or sinuses, symptoms and signs of orbital or cavernous sinus disease, or an ulcerating lesion of the hard palate or gingiva. |
| FUNGI Aspergillus spp., especially A. flavus, Mucorales such as Rhizopus arrhizus, Fusarium spp., Scedosporium spp., Alternaria spp. and rarely other fungi such as Schizophyllum commune. |
| GLOBAL BURDEN Approximately 5% of cases of invasive aspergillosis involve the paranasal sinuses, so ~10,000+ cases worldwide. In Europe and N. America, approximately equal number of mucormycosis cases, but up to 10 times the number in India, and possibly other localities (as many more proportionally in diabetic patients). |
| RISK FACTORS Haematologic malignancy, aplastic anaemia and myelodysplasia, uncontrolled diabetes mellitus (sometimes the first presentation and often in ketoacidosis), transplant recipients (stem cell and solid organ) and chronic steroid use. Controlled diabetes is not a risk factor. |
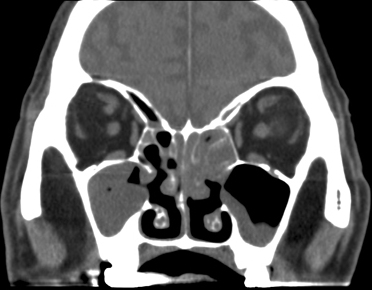
| DIAGNOSIS – EXAMINATION: nasal endoscopy shows dusky mucosa in early cases, but necrotic areas when more advanced. In neutropenic patients and those with diabetic ketoacidosis, these appearances are essentially diagnostic of acute fungal rhinosinusitis. In other patient groups vasculitis is the most common alternative differential diagnosis. – HISTOLOGY: frozen section analysis with simple H&E staining is about 85% sensitive compared with GMS-stained permanent sections. – CULTURES: more often positive from biopsy tissue if aspergillosis than mucormycosis. Surface swabs or other material found in the nose may be useful if pathogens other than A. fumigatus or A. niger are grown, as these organisms could be surface contaminants. – ANTIGEN: Galactomannan blood testing is positive in ~60% of acute Aspergillus FRS in haematology patients. Some patients have pulmonary or disseminated disease as well as rhinosinusitis, but most do not. – IMAGING: MRI is 15-20% more sensitive than CT for diagnosis, with peri-sinus invasion the most specific radiological feature. CT or MRI are useful for planning the extent of surgical debridement, and following progress, although the radiation exposure can mount up rapidly if CT is used. |
| TREATMENT Reversal of immune suppression is crucial, especially in diabetes and neutropaenia. Steroid dose should be minimised and serious consideration given to complete withdrawal of immunosuppression, even to the extent of losing a transplanted organ. GCSF and granulocyte transfusions may be important in therapy. Surgical or endoscopic biopsy and debridement are essential, but in neutropenic patients extensive debridement should be done once thrombocytopaenia has resolved to minimise the risk of catastrophic secondary haemorrhage after surgery. Voriconazole is the treatment of choice for invasive Aspergillus FRS. For rhinocerebral mucormycosis amphotericin B at high doses are necessary initially. For conventional amphotericin B this is ~1 mg/kg or higher, if tolerated. For lipid amphotericin B this is a minimum of 3 mg/kg and most physicians would use 5 mg/kg. Posaconazole is also active for both infections, and some rarer fungi, and has good results once the patient is able to take oral medication, and there are no absorption or drug interaction problems. Generally it is given after establishing control with amphotericin B and surgery in patients with mucormycosis. Hyperbaric oxygen has been used in some cases, with apparent benefit. |
| OUTLOOK ~50% of patients with invasive FRS survive. The highest survival rates are in diabetic patients, the lowest in those with uncontrolled leukaemia. Late diagnosis, extensive disease with evidence of extra-sinus tissue involvement and/or bony destruction were detected (~33%) is less favourable. Brain abscess and cavernous sinus thrombosis are especially difficult to treat. Selecting the correct antifungal agent initially is very important, as is adequate surgical debridement, sometimes requiring repeated debridements. Granulocyte transfusions have occasionally been used successfully, if neutropaenia is prolonged. |