Neglected tropical diseases (NTDs) are a diverse group of conditions of parasitic, bacterial, viral, fungal and non-communicable origin. They cause pain and disability, creating lasting health, social and economic consequences for individuals and societies. They prevent children from going to school and adults from going to work, trapping communities in cycles of poverty and inequity. People affected by disabilities and impairments caused by NTDs often experience stigma within their communities, hindering their access to care and leading to social isolation. It is estimated that NTDs affect more than 1 billion people, while the number of people requiring NTD interventions (both preventive and curative) is 1.6 billion.
Fungal NTDs are classed as mycetoma, chromoblastomycosis and other deep mycoses (including sporotrichosis)

Chromoblastomycosis
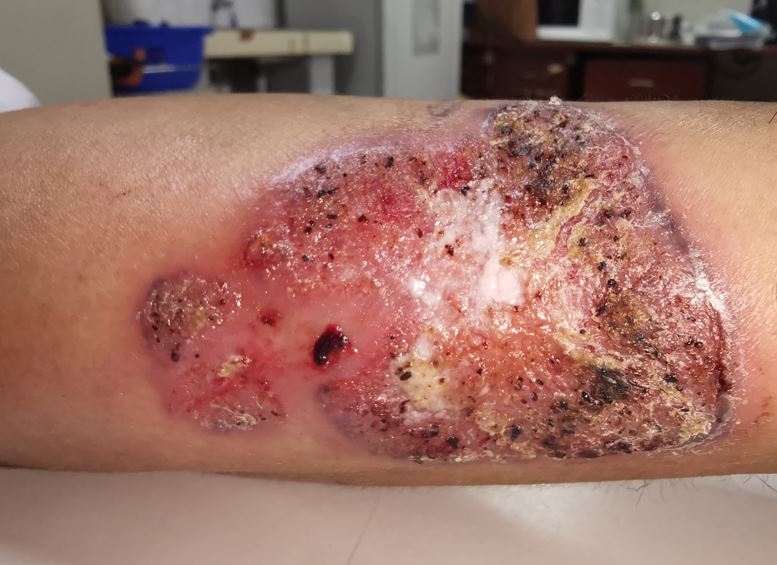
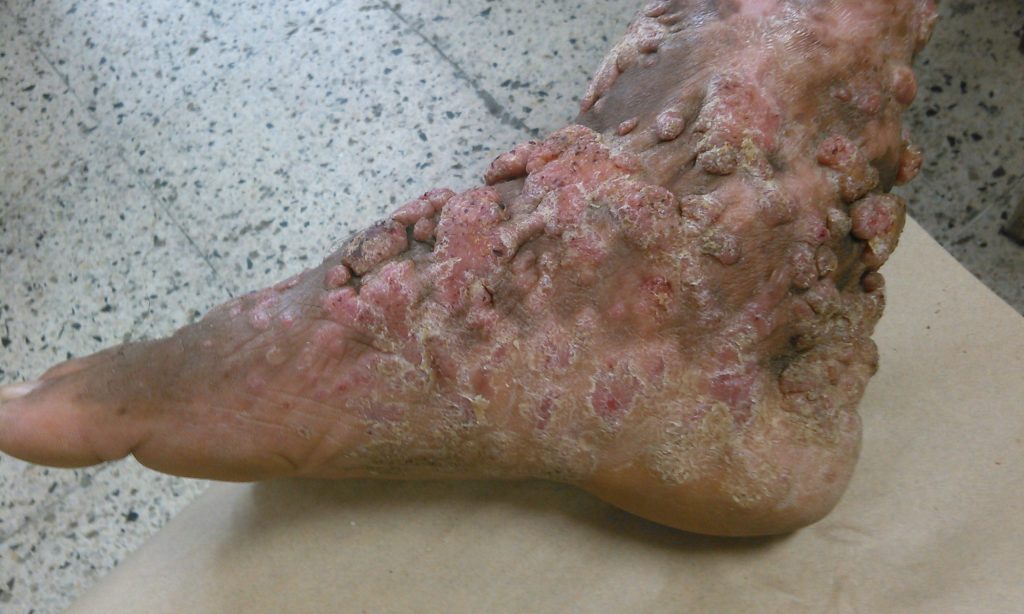
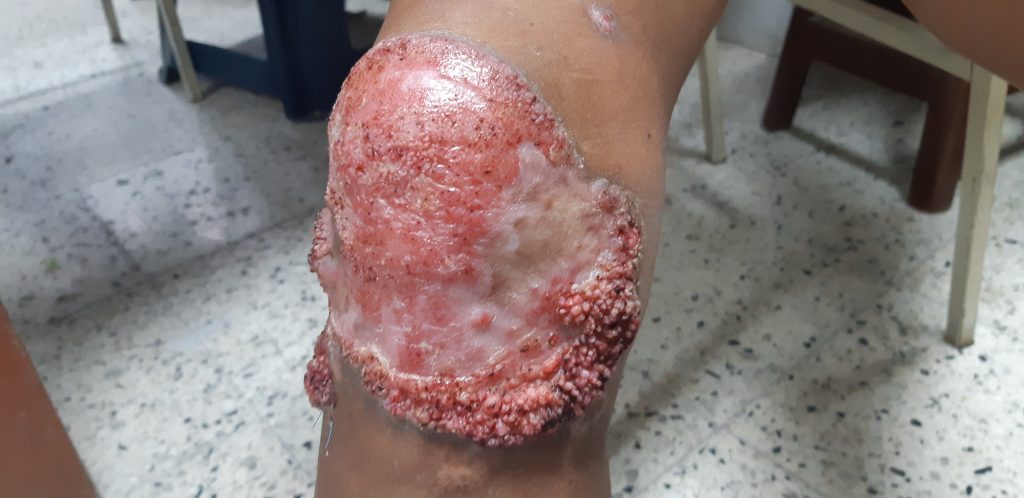
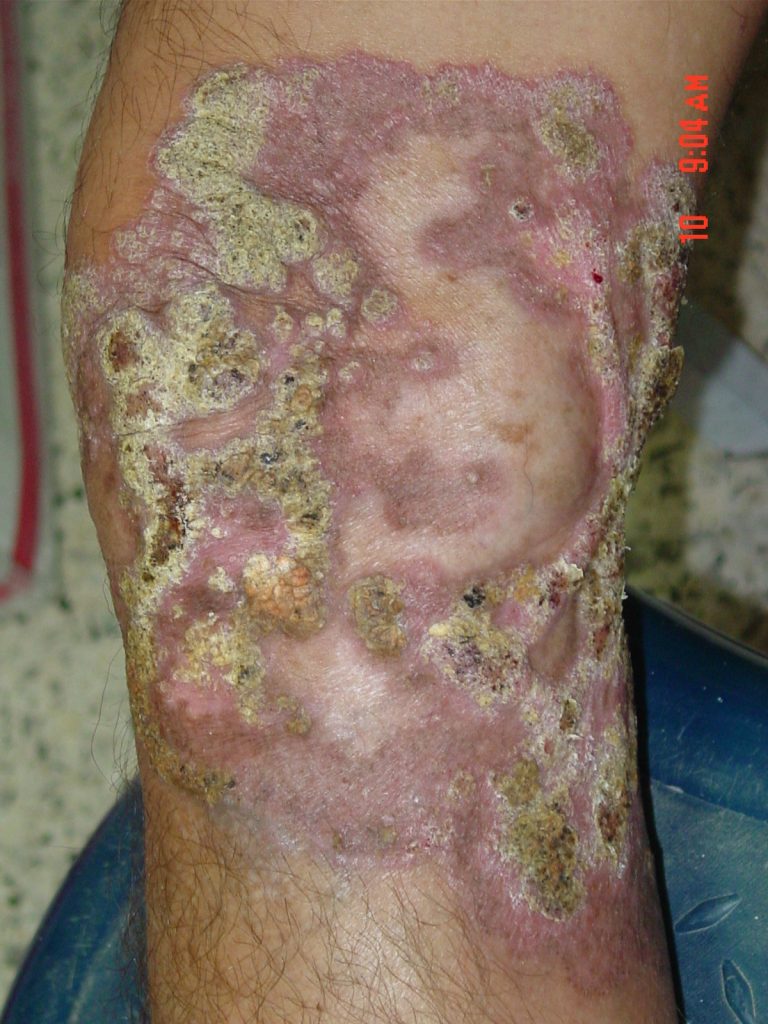
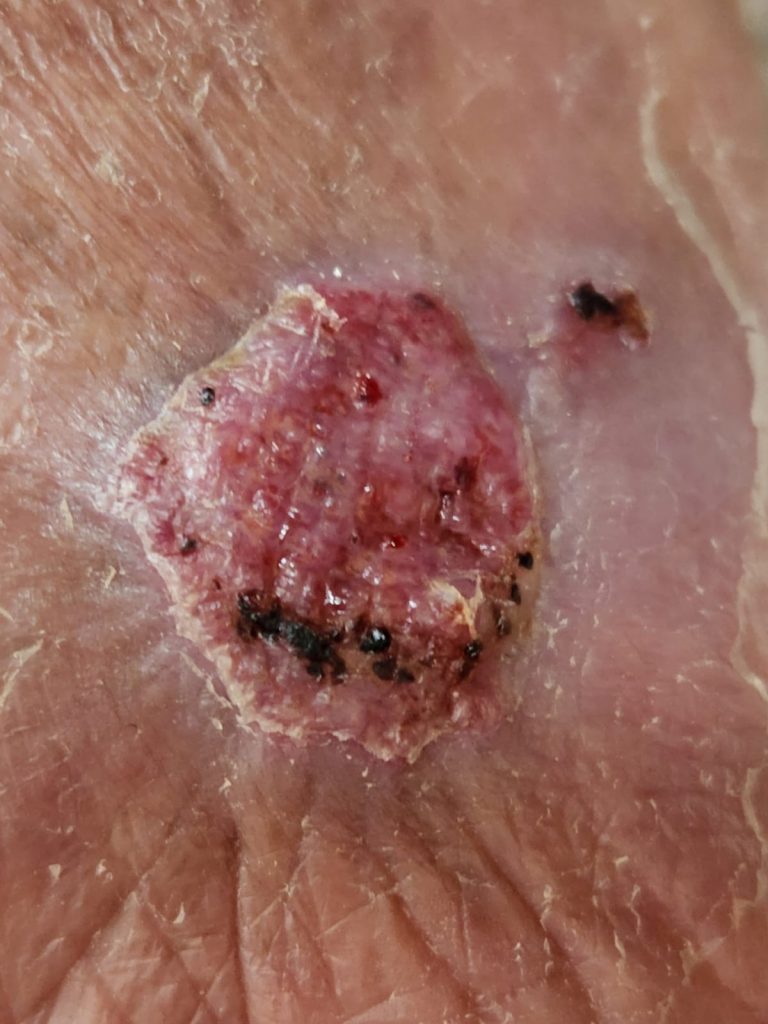
| OVERVIEW For reviews see Queiroz-Telles et al (2017), or read the detailed GAFFI factsheet Chromoblastomycosis (CBM) is a cutaneous and subcutaneous mycosis characterized by the appearance of proliferating chronic skin lesions following traumatic implantation of the fungus. Sites most commonly affected are the lower limbs. Upper limbs and buttocks are also frequently involved. Outbreaks on ear, face, neck and breasts have been occasionally reported. Lesions start out as a nodule or papule, that slowly enlarge becoming verrucose and wart-like. Old lesions can be tumorous or cauliflower-like in appearance. Lymphatic and hematogeneous dissemination have been described, but they are infrequent. |
| FUNGI Many melanised (black fungi) fungal species can be the etiologic agents of this disease. The most frequent are: Fonsecaea pedrosoi complex (includes F. monophora and the species formerly known as F. compacta) and Cladophialophora carrionii. Less common species involved are Phialophora verrucosa, Rhinocladiella aquaspersa, Exophiala spp and new Fonsecaea species. |
| GLOBAL BURDEN This condition occurs worldwide, but the frequency is much higher in tropical and subtropical areas of Africa, Central and South America, Asia and Australia. Global burden is unknown. In high endemic areas the incidence can reach 16 cases per 100,000 inhabitants. |
| RISK FACTORS This disease is occupational and relates to activities that can cause traumatic injury and contact with contaminated material. It is frequently observed in agricultural labourers. |
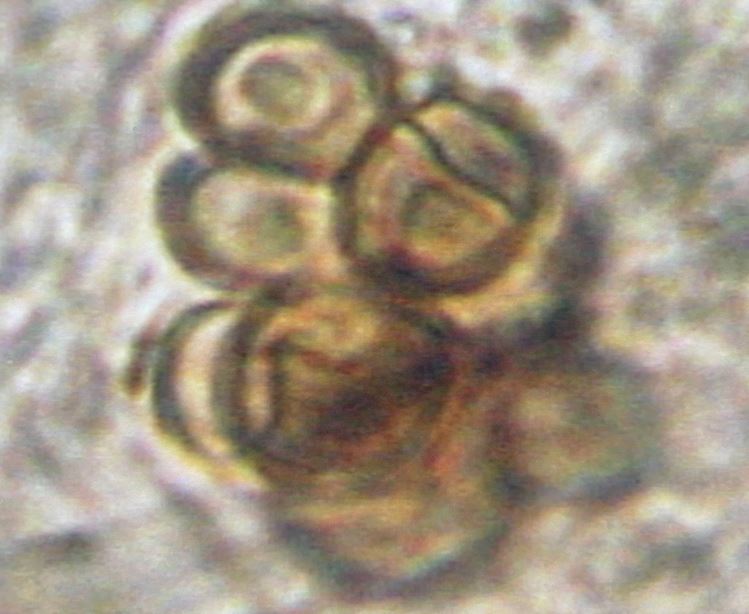
DIAGNOSIS |
| TREATMENT No optimal treatment has been identified, but swift diagnosis and treatment leads to a better rate of recovery. Many patients seek help after many years of living with this disease. Cryosurgery is an option when the lesions are small and the procedure has good outcomes. Itraconazole at 400 mg/day has been shown to yield a higher response than 200 mg, especially when the lesions are large. Patients usually improve, but a complete cure is rare. In addition, many cases require years of treatment, which is costly. In some cases, itraconazole combined with flucytosine has been used with good results. Terbinafine has been reported to have a similar success rate than that obtained with itraconazole. Posaconazole, 800 mg/day has also been used for the treatment of chromoblastomycosis with a success rate in refractory disease of 82% (from a small number of patients). |
| OUTLOOK Small and localized lesions have a good prognosis. Cure is difficult when the lesions are large. Most common complications are ulceration and secondary infections and lymphoedema. |

Sporotrichosis
| OVERVIEW Sporotrichosis can occur when fungus is implanted under the skin following minor trauma, such as handling thorny plants or a bite/scratch from an infected cat. Immunocompromised patients, and those with diabetes or alcoholism, are at increased risk of sporotrichosis developing into a life-threatening disseminated disease. The vast majority of cases of sporotrichosis have lymphocutaneous disease or localised ulceration of the skin, without nodules or lymph node swelling. Disseminated disease occasionally occurs with multiple skin nodules, osteoarticular disease, especially affecting large joints, and meningitis. Pulmonary sporotrichosis is also reported by rare, presenting similarly to subacute invasive pulmonary aspergillosis. See the GAFFI factsheet on sporotrichosis. |
| FUNGI Sporothrix schenckii complex (includes S. albicans, S. brasiliensis, S. globoa, S. luriei, S. mexicana and S. schenckii). [ teleomorph = Ophiostoma stenoceras ] Isolated from soil, wood and plant matter Read more at Dr Fungus |
| GLOBAL BURDEN Sporotrichosis has been reported worldwide, with most cases coming from Central and South America (Mexico, Colombia, Brazil, Peru) and parts of China. Hyperendemic rural areas may have attack rates of 1 case per 1000 of the population. In northern India, ~30% of inhabitants in villages where sporotrichosis had been reported had evidence of exposure to the organism compared with 6% in villages without clinical cases. Point source outbreaks have been know to occur. These have been traced to infected cats, certain mosses and hay. Please see the review by Chakrabarti et al (2014). |
| RISK FACTORS Farmers, gardeners and forestry workers are at increased risk of sporotrichosis. Those affected are usually healthy adults, under the age of 30, but young children can also be infected. S. schenckii most commonly enters the body through traumatic implantation, but only a minority of patients recall any history of trauma. AIDS may also lead to disseminated sporotrichosis. |
| DIAGNOSIS The best test to identify sporotrichosis is a skin biopsy with both histopathological examination and fungal culture. Aspiration can lead to false negative results, as organisms are scanty. Antibodies directed against S. schenckii may be detected in blood in those with disease, but are particularly valuable to diagnose meningitis. This is due to S. schenckii, as cerebrospinal fluid (CSF) cultures are invariably negative, but yield specific antibodies. Skin testing with Sporothrix antigen is usually positive in patients with this disease and may be a useful diagnostic tool (Bonifaz, 2018). |
| TREATMENT A saturated solution of potassium iodide and itraconazole is the treatment of choice. Side-effects of potassium iodide include metallic taste in mouth, salivary gland enlargement and rash. Terbinafine 250 mg twice daily is also highly effective. Fluconazole is less effective, as all isolates are resistant. Amphotericin B is initially useful for disseminated and meningeal disease, although micafungin may be more active, followed by itraconazole. Sporothrixio spp are resistant to voriconazole. In pregnancy, local heat (42-43ºC) application to the lesions, over several months, may be effective. |
| OUTLOOK Excellent for cutaneous and lymphocutaneous disease, with cure rates exceeding 95%. Meningeal and pulmonary sporotrichosis are difficult to diagnose and treat, with less positive outcomes. |

Mycetoma
| Disease name and synonyms Mycetoma; eumycetoma when caused by fungi, actinomycetoma when caused by bacteria. |
| Fungi responsible The most common fungal causative agents are Madurella mycetomatis, Madurella tropicana, Madurella fahali and Scedosporium apiospermum. |
| Disease description The disease is characterised by a painless subcutaneous mass, multiple sinuses and purulent or seropurulent discharge containing mycetoma grains. Grains are of various colours, sizes and consistent with the causative organism. The subcutaneous mass usually spreads to involve the skin and deep structures, resulting in destruction, deformity and loss of function – occasionally it can be fatal. In more than 80% of patients mycetoma affects the hand or foot. Occasional cases of head and neck, chest, abdominal wall, perineum or gluteal region are recorded. Rare mycetoma sites include the eye, sinuses, mastoid bone and scrotum. Eumycetoma has a slower progression than the more rapidly invasive actinomycetoma, but ultimately can be just as destructive. See the GAFFI factsheet on mycetoma. |
| Frequency and global burden The disease is endemic in many tropical and subtropical regions across the world, with high prevalence in the ‘mycetoma belt’. The belt stretches between 150⁰S and 300⁰N, and includes Sudan, Somalia, Senegal, India, Yemen, Mexico, Venezuela, Columbia, Argentina, and Iran, amongst others. There are probably between 20,000 and 50,000 cases worldwide based on literature reports. Most cases are reported from Sudan, Mexico and India.. |
| Underlying problems and at risk patients The most common age of infection is young adulthood (70% of the cases are between ages 11 and 40), with some children and older people affected. In most countries men are affected more than women. |
| Diagnostic testing Surgical biopsy is important to obtain grains for culture, molecular identification and histopathological examination. Individual grains have a distinctive appearance under direct microscopy, depending on causative agent, but this is insufficient to determine the bacteria or fungi responsible for the infection. Culture requires a range of media, including fungal, bacterial and mycobacteria plates and/or liquid culture. Years of experience are required to identify all of the fungi and bacteria that cause mycetoma, and there are many variants and isolates that resemble others. It is recommended to plate as many grains as possible in order to increase the chance of culturing the organism. Formal genetic identification using sequencing is most reliable. Susceptibility testing is not standardized and has not been well correlated with treatment outcome. Various imaging modalities are useful to define the extent of disease. Conventional X-ray, ultrasound to identify grains and MRI all have an essential place in determining the disease spread, and to establish a disease management plan. Currently, the available diagnostic tests and techniques are invasive, tedious and expensive. Most of them do not exist in endemic regions, and patients need to travel far to establish the diagnosis. |
| Treatment The treatment of eumycetoma involves a combination of antifungal treatment (currently itraconazole 400mg/day) and surgical excision. Excision ranges in extent from wide local excision to repetitive debridement, and in severe cases, amputation. Surgery is indicated for cases resistant to medical therapy and when the lesion is localised. It may be life-saving in advanced disease that is complicated by secondary bacterial infection, sepsis, massive bone involvement, and poor general condition. Some data indicate that voriconazole may be a better treatment for certain organisms, notably Medicopsis (Pyrenochaeta) romeroi. Eumycetoma treatment is prolonged with a low cure rate and high recurrence and dropout rates. |
| Outlook and prognosis Eumycetoma patients usually respond poorly to medical therapy. Improvement is slow and hard to evaluate, even after months of treatment. Many patients eventually fail to complete education or lose their jobs. For more information on actinomycetoma see Dermatology Advisor |
