For more information about CPA please see the Aspergillus&Aspergillosis website. For patient support and lifestyle information please visit Aspergillosis.org (Patients and Carers website).

In the UK, patients with the following signs of CPA can be referred to the National Aspergillosis Centre (based at MFT, Manchester)
- At least one pulmonary cavity on chest imaging with or without a fungal ball (aspergilloma) which has been present for at least three months and a positive aspergillus species test results by either serology or culture.

Clinical lectures
Surgical management of chronic pulmonary aspergillosis (CPA)
Managing chronic pulmonary aspergillosis (CPA)
Chronic pulmonary aspergillosis: global burden and diagnosis
Chronic pulmonary aspergillosis: Dangerous gaps in diagnostics & treatment (GAFFI interviews)
Chronic pulmonary aspergillosis in a resource-limited setting by Prof Wahyuningsih
How to interpret Aspergillus antibody (IgG) titres for chronic aspergillosis

| NAME(S) CPA, chronic pulmonary aspergillosis, aspergilloma, chronic necrotizing pulmonary aspergillosis |
| DISEASE The term CPA embraces several closely related disease entities including simple aspergilloma, chronic cavitary pulmonary aspergillosis (also known as complex aspergilloma) and chronic fibrosing pulmonary aspergillosis. CPA is a slowly progressive and destructive disease of the lungs, usually of one or both upper lobes, with cavity formation the most common radiological feature. It is arbitrarily defined as being present for at least 3 months. It occurs in non-immunocompromised or minimally immunocompromised patients. Some patients have nodules, which probably represent early disease, and may be mistaken for lung cancer, and have a positive PET scan. Common symptoms are fatigue, weight loss breathlessness, productive cough and haemoptysis (coughing up blood). The disease is often mistaken for pulmonary tuberculosis and both diseases can co-exist. About 25% of patients have an aspergilloma (fungal ball) present, the remainder one or more cavities and/or nodules. |
| FUNGI Typically Aspergillus fumigatus, rarely A. niger or A. flavus. |
| GLOBAL BURDEN CPA is estimated to affect over three million people worldwide, of whom ~1.2 million have had tuberculosis. |
| RISK FACTORS Most commonly TB, COPD, sarcoidosis, allergic bronchopulmonary aspergillosis, prior pneumothorax, prior lung cancer (sometimes with lung radiotherapy or surgery) and asthma (including SAFS). Most patients are not taking corticosteroids or other immunosuppressant drugs, but many are on inhaled corticosteroids or take small doses of oral corticosteroid. Many patients have low gamma-IFN responses to standard stimuli. |
| DIAGNOSIS The key diagnostic tests are serum Aspergillus IgG (AKA precipitin), and radiology showing one or more cavities or nodules. Aspergillus fumigatus IgG antibodies are detectable in ~90% of patients; alternative approaches to diagnosis include detectable A. flavus or A. niger IgG antibodies, A. fumigatus IgE antibodies and biopsy/excision of lesions showing hyphae consistent with Aspergillus within a cavity. Sputum culture positive rates are ~25% and Aspergillus PCR is more sensitive, but many patients are still negative. |
| TREATMENT Oral itraconazole and voriconazole yield a 60-80% response rate, although it can take some months for full benefit. Response only occurs if blood levels of antifungal are in the therapeutic range. Twelve months of therapy (with itraconazole) substantially reduces the risk of relapse after stopping treatment, compared with six months of treatment. Second line therapy with posaconazole is useful for those who fail or cannot tolerate itraconazole or voriconazole. Fluconazole is ineffective, IV amphotericin B and micafungin also yield a 60% response rate, of limited duration. Surgical excision of simple aspergillomas. For symptomatic patients and those with radiological progression, oral itraconazole, voriconazole or posaconazole. Rescue or primary therapy with micafungin or amphotericin B is an alternative. A few patients have benefitted from gamma IFN therapy. |
| OUTLOOK CPA progresses at a variable rate and is often diagnosed late. Severe disease carries a 15-30% mortality in the first 6 months after diagnosis. Death is mainly due to pneumonia and lung bleeding. Those with minor involvement will do well for many years, if progressive lung destruction can be halted. Azole resistance in A. fumigatus is becoming an increasing problem, especially in patients with aspergillomas and those with low serum levels of itraconazole. |
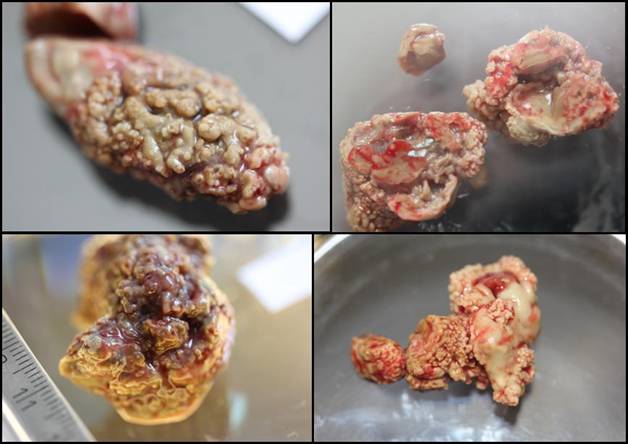
Surgically-removed aspergillomas (fungal balls) 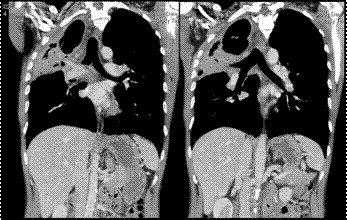
CT slices showing one large and some smaller cavities in the right upper lung, surrounded by marked pleural fibrosis 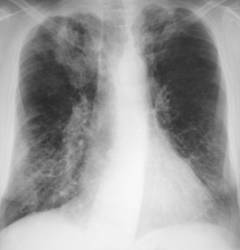
CPA complicating ABPA 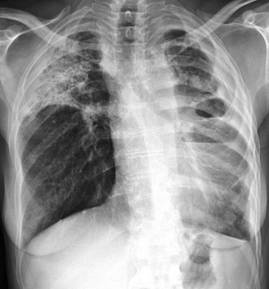
Severe bilateral CPA with the left upper lobe replaced by one large and several smaller cavities and a fluid level (which on aspiration grew a pure growth of Aspergillus fumigatus). There is also extensive disease of the right u
